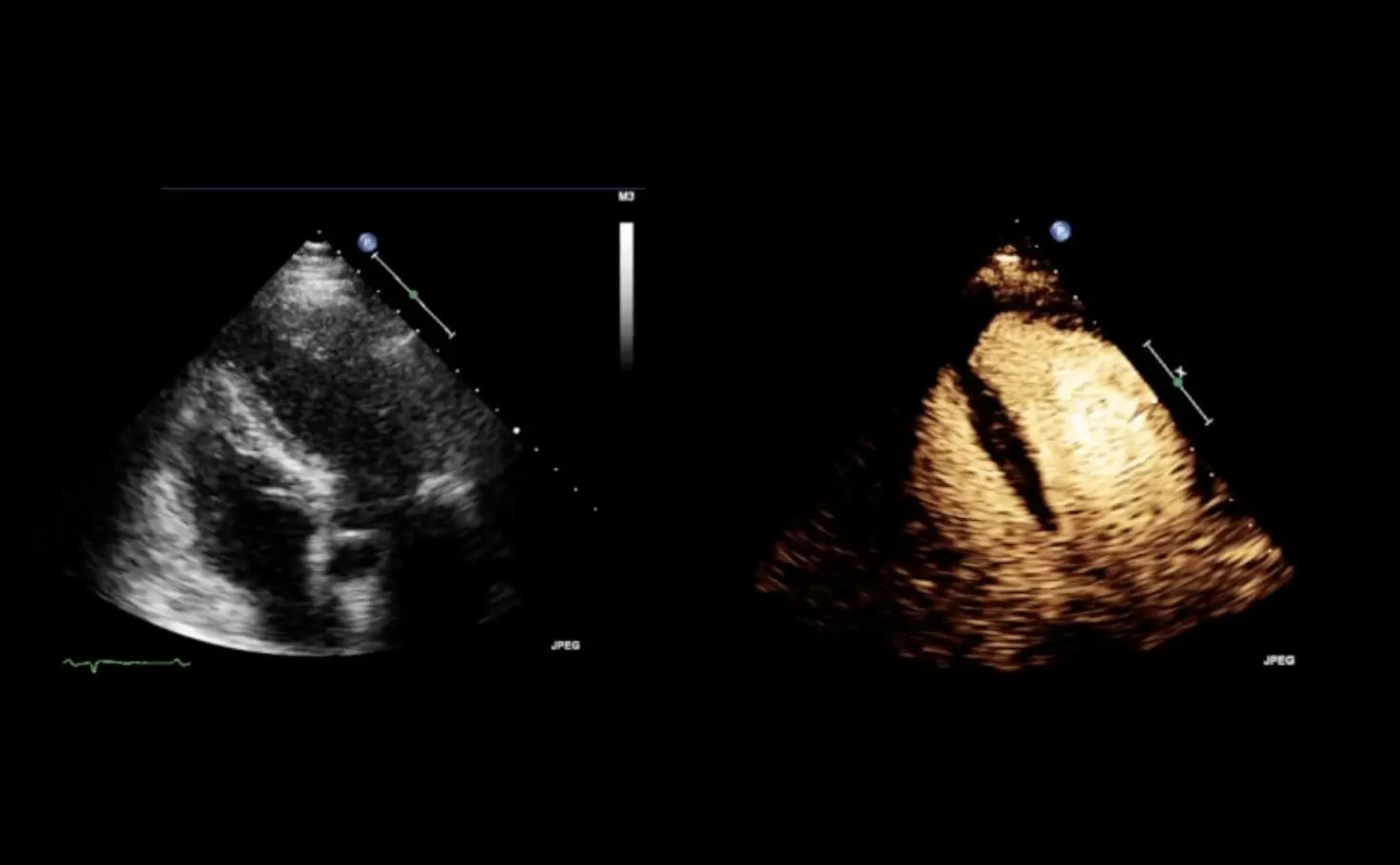
Diagnosis is the first step in the adequate management of patients and a key aspect of healthcare: diagnosis allows for an understanding of a patient's particular health condition and guides subsequent healthcare decisions. Achieving a correct diagnosis allows the physician to choose the most adequate therapy. While ultrasound is often the first imaging examination, assessment of the perfusion pattern and lesion characteristics requires the use of a contrast-enhanced imaging examination. Therefore, the patient is frequently referred to a CT or MRI follow-up examination. In the early 2000’s the advent of second-generation ultrasound contrast agents gave the opportunity to get information about tissue perfusion and vessel display that was not possible during unenhanced ultrasound exams, leading to more specific lesion characterization1-3. This can save resources4 and allows immediate assessment of doubtful lesions not characterized during baseline ultrasound.
Moving towards value-based healthcare
A value-based healthcare model is being increasingly advocated as part of a modern approach to patient management5. This model refers to a framework that can improve individual patient health outcomes when measured per unit of expenditure and has been proposed by a joint statement from leading radiological societies in Europe, the USA, Canada, Australia, and New Zealand5. It is now recognized that radiology is a key component of healthcare that has an enormous impact on patient outcomes, and as such is a vital element of value-based healthcare. By embracing the principles of value-based healthcare, radiology can contribute to the adoption of a value-driven system, where all investigations or interventions contribute positively to patient outcomes5. One of the pillars of value-based healthcare is achieving the best possible outcomes using the available resources.
About contrast-enhanced ultrasound
CEUS has become an established diagnostic modality in liver and cardiovascular imaging2,3. Unenhanced ultrasound examinations may sometimes identify abnormalities that may require further investigation. For example, it may identify focal liver lesions that require further assessment to differentiate benign from malignant lesions4. An important aspect to consider when selecting an imaging test is the ability to provide a rapid diagnosis. CT and MRI usually require referral with associated wait time and may be contraindicated in some patients. CEUS may be used to enhance lesion vascularization and therefore distinguish between benign and malignant liver lesions. Moreover, CEUS can be performed during the unenhanced ultrasound session, leading to a diagnosis that is potentially more rapid.
The value of contrast-enhanced ultrasound
CEUS has been shown to provide complementary diagnostic performance to other imaging modalities such as contrast-enhanced CT or contrast-enhanced MRI for the assessment of focal liver lesions4. The use of CEUS instead of contrast-enhanced CT has been considered cost-effective in the surveillance of cirrhosis and the characterization of incidentally detected focal liver lesions4. CEUS may thus be cost-saving compared to techniques such as CT and MRI in some instances4.
Contrast-enhanced ultrasound in routine practice
Although other imaging diagnostic procedures are commonly performed, ultrasound remains a widely used technique for a large range of clinical applications, available in almost every clinical unit. Indeed, it has been suggested that whole-body ultrasound is suitable for a number of assessments6. In fact, point-of-care ultrasound has been considered as the new fifth pillar of physical examination, building on inspection, palpation, percussion, and auscultation. It has been considered that “ultrasound devices are now as portable as the stethoscope and have the ability to look beyond the chest therefore, the term whole body ultrasound (WHOBUS) would more appropriately describe the potential of bedside ultrasound”4. In this regard, CEUS can bring added clinical value in the assessment of focal liver lesions, and breast lesions, during cardio-vascular examinations or ultrasonography of excretory urinary tract in pediatric patients. Given its wide range of applications and fast diagnostic results, CEUS has the potential to save valuable resources with economic benefits as well as advantages for the clinician and patient.
The advantages of CEUS
CEUS can significantly improve the ability of ultrasound to characterize hepatic and breast lesions. Numerous scientific publications have demonstrated the clinical value and the diagnostic performance of CEUS exams in liver and cardiac imaging2,3 and its cost-efficiency4 compared to more costly imaging techniques such as contrast-enhanced CT or MRI. Given these potential benefits, CEUS can be considered an established part of radiological imaging and an important component of value-based healthcare.
1 Strobel D et al. Contrast-enhanced Ultrasound for the Characterization of Focal Liver Lesions -Diagnostic Accuracy in Clinical Practice (DEGUM multicenter trial), Ultraschall in Med 2009: 376 -382
2 Dietrich C. et al. Guidelines and Good Clinical Practice Recommendations for Contrast-Enhanced Ultrasound (CEUS) in the Liver-Update 2020 WFUMB in Cooperation with EFSUMB, AFSUMB, AIUM, and FLAUS, Ultrasound in Med. & Biol., Vol. 46, No. 10, pp. 2579-2604, 2020
3 Senior R. et al. Clinical practice of contrast echocardiography: recommendation by the European Association of Cardiovascular Imaging (EACVI) 2017, European Heart Journal -Cardiovascular Imaging (2017) 0, 1–33
4 Westwood M, Joore M, Grutters J, et al. Contrast-enhanced ultrasound using SonoVue® (sulphur hexafluoride microbubbles) compared with contrast-enhanced computed tomography and contrast-enhanced magnetic resonance imaging for the characterisation of focal liver lesions and detection of liver metastases: a systematic review and cost-effectiveness analysis. Health Technol Assess. 2013;17(16):1-243
5 Brady AP, Bello JA, Derchi LE, et al. Radiology in the Era of Value-Based Healthcare: A Multi Society Expert Statement From the ACR, CAR, ESR, IS3R, RANZCR, and RSNA. J Am Coll Radiol. 2021;18(6):877-883.
6 Denault A, Canty D, Azzam M, et al. Whole-body ultrasound in the operating room and intensive care unit. Korean J Anesthesiol. 2019;72(5):413-428.